Self-Esteem
In This Article
Click to jump to your selected section.
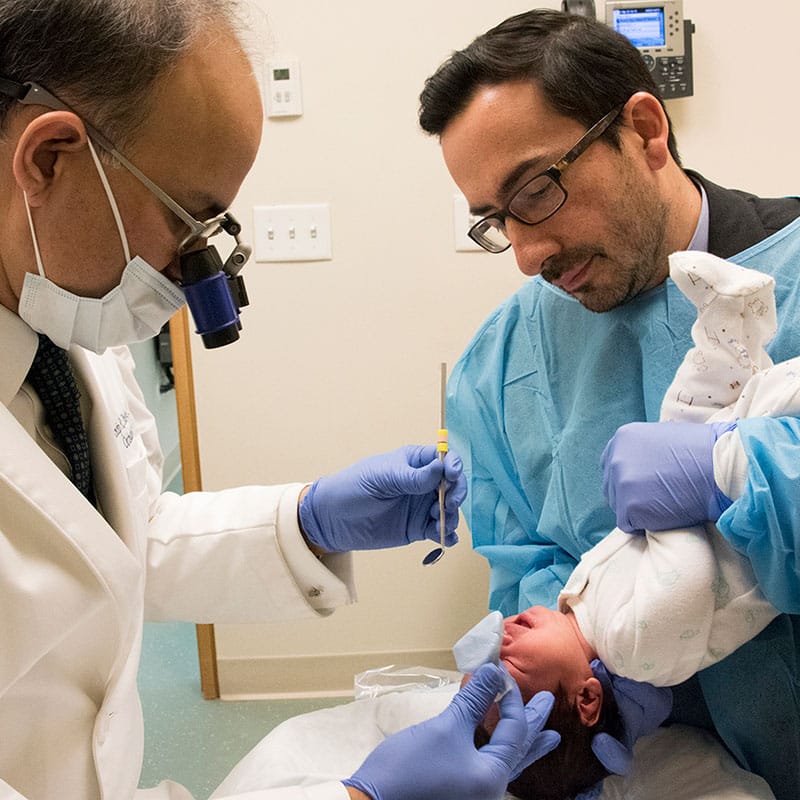
What is Cleft Lip and/or Palate?
Prevalence
Causes
Types of Cleft Lip and/or Palate
Diagnosing
Treatments & Procedures
Living with Cleft Lip and/or Palate
Potential Complications and Challenges
Meet a Member of the myFace Community
Support for People Living with Cleft Lip/Palate
Resources for the Craniofacial Community
What is Self-Esteem?
Self-esteem refers to how much people accept and value themselves. It reflects one’s sense of self respect and self-worth.
Factors That Affect Self-Esteem
People tend to base much of their self-esteem on how physically attractive they are to themselves and to other people. This is primarily because society places a great deal of emphasis on physical attractiveness. Today’s popular culture is filled with images that promote the goal of physical perfection and beauty. We are encouraged to buy products that claim to beautify the users. We are persuaded to believe that if we look like the model in the ad, we will like ourselves better, attract more friends, and be regarded by others as more appealing.
During childhood, young children begin to compare themselves to others and to notice differences. They become concerned that they are too tall, too short, too fat, or too skinny. During adolescence, teenagers also focus on fitting in and being accepted by their peers. They feel the need to look, dress, or act a particular or accepted way. Most children and teenagers struggle at some point with fitting in or trying to attain often impossible-to-achieve standards of beauty. For children with facial differences and their families, this struggle is often complex and emotionally challenging.
People’s body image and sense of physical appearance contribute to their development of self-esteem. Children who have multiple surgeries on their face may believe that there is something wrong with their appearance. As a result, they may develop low self-esteem.
Because of society’s emphasis on an attractive appearance, people may react negatively to children with facial differences. For example, people may look away or avoid eye contact. As children with facial differences get older, they may become more aware of being viewed negatively by others. This negative perception may influence their sense of self-worth. Teasing, exclusion, and verbal and non-verbal insults by others may also contribute to a child’s development of low self-esteem.
Primary caregivers (parents, guardians, and others who have a major responsibility in caring for the child) play an especially strong role in determining whether or not a child will develop high self-esteem. How they perceive and respond to the child highly influences a child’s body image, overall self-image, and sense of self-worth. At a very young age, children sense their caregivers’ attitude towards them. Children are keenly tuned into their parents’ feelings.
Children’s feelings about their facial differences and about themselves, therefore, are usually the result of:
• The caregivers’ reaction to and ability to cope with the child’s appearance.
• The reactions of other people, including siblings, relatives, and adults and peers outside the family.
• The child’s physical differences.
• The reconstructive surgical process.
These feelings affect a child’s self-esteem. Children with low self-esteem may feel inferior, worthless, and sad. These feelings may, in turn, affect a child’s emotional well-being, development, and ability to get along with others.
Self-Esteem and Coping Skills
Coping is the manner in which people respond to difficulties in their lives and the actions they take to overcome these problems. Children’s coping skills are put to the test when they begin to interact with other people at school and in other social settings. Self-esteem and coping skills are often related; children with low self-esteem tend to develop poor coping skills. Those with positive self-esteem have developed helpful coping mechanisms.
Effective and ineffective coping skills:
• Denial – Denial means ignoring a problem or pretending that it does not exist. It is one of the most common ways that children cope with unpleasant things. For example, children may exhibit denial when they view their facial differences as less severe than others do. Some denial may be healthy, as is the case when children are aware of their facial differences, but choose not to focus all of their attention on it.
• Anger – Anger is a negative emotional response to an unpleasant situation that can result in a verbal and/or physical reaction or just be felt. It is an emotion that may be difficult to understand in children. On the positive side, anger can motivate children to speak up or act in ways that assert their ideas or needs. However, uncontrolled anger may lead to behavior that pushes other children or family members away or brings on excessive criticism (see Acting Out). It is important to consider anger in the context of the situation in which it occurs. When a child is angry, parents should consider the circumstances, the appropriateness, and the degree of control.
Most parents would prefer that their child talk about feelings of anger instead of act on them. This is not always easy for children to do. Children often express themselves non-verbally. Parents can help their children identify feelings by using story books, role playing, and encouraging them to talk about their feelings. When anger becomes intense, it may be difficult for a child to hold it inside or to express it in a useful way. Expressing anger in a way that is not constructive is a behavior we call “acting out.”
• Acting Out – As defined above, acting out is expressing strong feelings in a way that can be emotionally, verbally, or physically abusive. It often results in negative attention. Although acting out usually is thought of as negative behavior, at times it may be an appropriate and important expression of anger. Thinking of acting out behavior as telling us something important about how children are feeling can allow parents to better understand their children and more effectively help them feel better.
• Depression – Depression includes feelings of sadness and decreased interest and pleasure in activities. Symptoms of depression vary with age and with one’s unique personality. The American Academy of Child and Adolescent Psychiatry recognizes depression as an emotional disorder when the feelings of depression persist and interfere with a child or adolescent’s ability to function. Children who have experienced early losses, have academic challenges, or have emotional or behavioral difficulties are at higher risk for depression than other children.
In general, symptoms of depression in children may include frequent sadness or crying, decreased interest in previously enjoyed activities, social isolation, feelings of hopelessness, extreme feelings of guilt, irritability, moodiness anger, withdrawal, complaints of physical illness such as headaches and stomach aches, poor concentration, a major change in sleep and eating patterns, talk of or efforts to run away from home, and thoughts or expressions of suicide or self-destructive behavior. Depressed younger children may pretend to be ill, refuse to go to school, cling to a parent, or worry that a parent may leave them or die. Depressed older children may be moody, get into trouble at school, isolate themselves, and feel chronically misunderstood by others, especially by adults.
Parents should allow their child to experience some unpleasant emotional feelings. Every child must learn to cope with feeling sad, bored, angry, or discouraged at times. However, parents who believe their child is experiencing symptoms of depression should inform their craniofacial team, which can provide a referral to a child/adolescent mental health professional.
• Social Skills – Social skills are developed at an early age within the family context and, later, in social settings such as school or camp. Children’s social skills are often influenced by their personality and coping mechanisms. Some children are naturally outgoing and can easily start a conversation with others, while other children are shy and may only speak when spoken to. Parents can help their child develop a range of social responses to others that help the child feel more self-assured and comfortable in social situations. It is important for children to know how and when to respond to hurtful remarks. Practicing well thought-out responses to potentially difficult social situations can help a child cope with the situation if it does occur (see Teasing and Bullying).
• Making Choices – People feel more self-confident and less helpless when they have some control over what happens to them. As children get older, it is important for parents to involve their children in making their own choices about their lives, even if those choices are about simple issues. For example, allow the child to schedule a surgery during the summer if the child does not want to miss school activities.
• Taking Risks – Parents of children with facial differences may worry about their child being injured physically (perhaps while wearing a distraction device or just after a surgical procedure) or emotionally by being rejected by their peers. When children are overprotected, they often sense that their parents do not believe that they are capable of doing things without help or that they cannot stand up for themselves. Parents can help their children in important ways by believing in them and having confidence in their ability to handle themselves, even though they may make mistakes. This will help them develop confidence in their own judgment and abilities and build their self-esteem.
In addition, children who are overly protected because of their medical condition may grow up to feel that they are entitled to special treatment from others. If they do not get this special attention, they may become disappointed and angry, and in turn, may blame others for their bad feelings. It is very important to challenge children to do all they can for themselves.
Parents can bolster their child’s self-esteem by praising their child for being strong and handling a difficult situation or surgery. It is okay for parents to buy a child a gift before surgery. However, too much spoiling through gift giving or making promises can contribute to a demanding child who may develop unrealistic expectations of others later in life. Some parents encourage children who receive many gifts to donate some of their gifts to children in need.
• Reconstructive Plastic Surgery – Reconstructive surgery may be intended to improve function, appearance, or both. While there have been major advances in the field of reconstructive plastic surgery, surgery is only one approach to improving a child’s self-esteem. Parents can help their child anticipate what to expect from surgery and understand the limitations of surgery. This includes developing a realistic expectation of how much of a change one can expect from a given procedure as well as understanding at what point surgery may not make a noticeable or positive difference. Older children may decide that they are comfortable with their appearance and that they do not want more surgery. Keep in mind that children’s perspectives as teenagers will likely differ from their views as adults. An added concern when deciding whether a child should have an optional procedure is that children may only be covered by their parents’ health insurance policy until the age of 18. Therefore, surgery may be more affordable as a child than as an adult.
Developmental Issues and Self-Esteem
When trying to determine how to improve the self-esteem of a child with a facial difference, parents need to be aware of certain developmental issues. Parents should know what is considered normal development, as well as the range of normal behaviors, attitudes, and thoughts for children at various stages of development. It is important to note that not all social, behavioral, or academic issues should be attributed to a child’s facial difference. Some issues may be associated with normal developmental stages while others may be attributed to a condition-related problem.
Infants and Toddlers (Birth – 2 years) – During their first two years, infants and toddlers begin to “attach” to their parents and to develop their sense of trust and overall feeling of security. Attachment is the process by which parents and children bond and parents learn to tend to their infant’s physical and emotional needs by feeding, holding, and soothing the child. This process is very important for a child’s emotional development. Infants and toddlers generally do not understand their medical condition. They tend to experience pain, restriction of motion, and separation from parents as challenges to developing their sense of trust and security. Hospitalizations may disrupt a child’s attachment process. Parents can facilitate the attachment process by participating in as much of their child’s care as possible while the child is hospitalized.
Pre-School Children (3 – 5 years) – During their pre-school years, children begin to develop a sense of independence. At this stage, children with special needs may start to partially understand their medical condition. For example, pre-school children may understand what it means to feel sick but not what causes the sickness. Their perspective tends to be limited to the way things appear in the moment. In addition, young children who attend pre-school or daycare interact with peers early on in their lives. As children begin to make comparisons between people or notice differences, issues of self-consciousness regarding physical appearance may emerge.
Early School-Aged Children (6 – 8 years) – During their early school years, children have an even clearer understanding that they are different from their peers or siblings. They may notice that they are receiving special treatment from parents, teachers, and caregivers. They may start to ask the question “Why me?” They may be able to describe reasons for illness, but their reasons may not be logical. Children at this age often engage in magical or supernatural thinking. They may believe they caused their facial difference by thinking bad thoughts or by fighting with their parents or siblings. At this age, children are mostly concerned with “being normal” and “fitting in.” They tend to think of differences as negative qualities. Children with facial differences may begin to internalize the thought that they are “not as good” as children without facial differences. They may come home from school angry or withdrawn after being teased or rejected by a peer.
Dealing with these developmental issues is a process for all children that extends into adulthood as people begin to accept themselves and learn to appreciate their strengths and acknowledge their weaknesses. Parents can help their school-age child with facial differences by providing encouragement, spending time doing activities with their child, and speaking with their child about how to best respond to teasing and rejection from others (see Teasing and Bullying).
Older School-Aged Children (9 – 12 years) – Children between the ages of 9 and 12 are better able to understand their medical condition and treatment, but their understanding is still limited. At this stage, children may begin to dislike things about their physical appearance. They may become self-conscious around others. Children may feel left out if they miss school or activities when they have a doctor appointment or are recovering from a surgery. Issues around differences and the importance of social acceptance outside of the family begin to emerge. Parents may need to restrict their child’s activities for medical reasons. However, parents can help children find creative ways to connect with their peers by writing cards, emailing, or having play dates.
Adolescents (13 – 17 years) – Teenagers are most concerned with issues of identity and fitting in with a peer group. Adolescents go through rapid physical changes, including growth spurts and hormonal changes that may impact the appearance of facial bones and features. Self-image and attractiveness to others become very important during adolescence. Self-confidence can decline when a teenager’s appearance is altered by a facial condition. Teenagers who are different in any way can find their years in high school to be emotionally challenging. For adolescents with facial differences, these challenges can be particularly intense. In a positive light, children at this developmental stage are also concerned about fairness and being a good person. Therefore, peers may be more open emotionally to people they perceive as different from themselves.
Late Adolescence and Early Adulthood (18 – 25 years) – During their late teens and early twenties, people’s attitudes and values go through many changes. While some adolescent attitudes may persist, older adolescents and young adults often become more tolerant and accepting of differences. This is a time when people begin to focus less on appearance and to expand their social circles to include peers with whom they have shared interests. In addition, young adults start to let go of the anger or insecurities they may have experienced in the past as they begin to value their own strengths and accomplishments.
How to Help Children of All Ages Develop Positive Self-Esteem
It is very important for parents to help their child feel good about himself or herself. Tips on how to help children develop positive self-esteem are as follows:
1. Self-esteem starts with your child receiving positive messages from you.
2. Compliment your child when he or she does something well or makes an effort.
3. Children need to be told that they are loved and valued for themselves, not just for their achievements. Do not limit praise to times when your child is successful at something.
4. Try to reward good behavior and focus less on punishment for bad behavior.
5. Point out something positive before criticizing or giving negative feedback to your child.
6. Be flexible about how your child does things and encourage your child to come up with his or her own solutions.
7. Set realistic goals and expectations for your child. Help your child learn how to cope with disappointment by occasionally allowing him or her to experience failure.
8. Talk with your child about how he or she is special and valued and provide examples.
9. Show satisfaction and talk about your own achievements. This gives your child permission to be happy with his or her own achievements.
10. Become aware of your own attitude toward people’s appearances, and if need be, tone down comments. Parents who make either positive or negative comments about looks send a message that physical perfection is important. Talk about attributes other than appearance.
Some other helpful hints:
1. Try not to overprotect your child even though it may result in your child feeling uncomfortable or unhappy at times. To grow and develop emotionally, it is important for children to learn how to bounce back from disappointments.
2. Treat children’s daily distresses as expected and without alarm to discourage them from turning small things into big things. Deal with problems by staying calm and suggesting useful solutions.
3. Help your child appreciate differences in him or herself and others. Provide your child with opportunities to be with other people who are different from him or her culturally, physically, and racially.
4. Connect your child with another child or group of children with facial differences so that your child can see that he or she is not the only one with a facial difference. Ask your doctor for contact information for another family, join an online group, or check out a Children’s Craniofacial Association retreat (http://www. ccakids.org/).
Self-Esteem and the School Setting
In the school setting, children with facial differences may encounter pressures and challenges that can affect their self-esteem. Parents should know about these challenges so they can help their children cope.
Special Issues – In the school setting, children may encounter both learning and social pressures. While not all children with a facial difference have learning problems, some may experience problems with speech, communication, hearing, vision, fine and/or gross motor skills, as well as other physical challenges.
Teasing and Bullying – The teasing and bullying that occur in a school setting is difficult for everyone, but it can be particularly difficult for children with facial differences. Teasing is most common during the elementary school years (grades one to five or six). Developmentally, this is a time when children want to fit in and be like their peers, so differences become a target for teasing. In addition, new social settings can be particularly hard for children with a facial difference. Therefore, teasing may occur when children make transitions from one grade to the next or from one school to another.
Because teasing and bullying of all children has become a national concern, many laws and school interventions are now being implemented to address the problem. For example, some schools have developed peer mediation groups that are often facilitated by school counselors. At some schools, children can fill out a Request for Assistance Report if they see another child pushing, gossiping, or picking on another student. If a child is caught bullying three times, the class determines a punishment that may include Saturday detention or eating lunch alone for one week. Other programs to cut down on teasing and bullying include, “Don’t Laugh at Me,” instituted by the New York-based non-profit agency Operation Respect (see Recommended Reading List for contact information). Some programs go beyond bullying to help more isolated children get involved in group activities and provide support groups on various topics including self-esteem, stress, and anger management.
To help eliminate teasing and bullying parents should:
1. Get involved! If your child’s school does not have policies on teasing and bullying, you can suggest them.
2. Schedule a meeting with your child’s teachers, principal, and counselor and then keep them informed of any problems your child experiences. The school staff may not be aware of the extent of the problems.
3. Volunteer to work with your child’s school on programs to increase awareness about differences. Parents of a younger child may present information about facial differences to their child’s class. Often a child’s classmates are curious and lack information. Once classmates have a better understanding of the medical condition, they are often less fearful, more accepting, and less likely to tease or bully the child. 4. Teach your child how to be assertive and practice with him or her. Sometimes a child will need help with developing a plan for confronting a bully. Practice ways to respond to someone who is teasing or bullying.
Examples of responses are as follows:
“We can still play together. I’m just like you in other ways.”
“Everybody’s different in some way.”
“I was born this way and my doctors are helping me.”
How to help children develop good self-esteem in school
To help children with facial differences develop resilience and good self-esteem despite the extra pressures of school, parents can do the following.
1. Prepare for all transitions into school, including to new teachers or grade levels, by visiting your child’s new teacher or school in advance. If you anticipate a difficult transition, talk with the school principal. The principal may be able to match your child with the teacher best qualified to address your child’s needs. Meet with school staff upon your child’s entry into a new school, and schedule a follow-up visit soon after school starts. Meet with your child’s teacher periodically. To prepare younger children for transitions to a new school year, talk with them about the activities and routines at the new school. Consider arranging play dates with some new classmates before the school year begins.
2. Be actively involved in your child’s school activities. As early as pre-school or nursery school, serve as a parent volunteer. In addition, you may be able to visit the classroom to demonstrate a skill or present information on a special issue, such as your child’s facial difference.
3. Continue to participate in your child’s education when your child moves on to middle and high school. Attend your child’s extracurricular activities and school performances, and seek opportunities in which you can be involved.
4. Help your child with homework as needed by assisting with time management and setting priorities. You may also help your child reduce stress and anxiety by helping your child set realistic limits on extracurricular activities.
5. Share your concerns with appropriate school system personnel. You may want to get involved with your local school board to influence policies regarding issues such as philosophy of education, curriculum, homework, school safety, equipment needs, special needs, and use of technology.
6. Be aware that your child may not always tell you when something negative is happening at school. Contact your child’s teachers and ask about how your child is doing and how your child is getting along with peers. Your child may need help with this problem, but not want to admit it or burden you.
7. Be realistic and honest with your child so that your child will be open and honest with you. It is not realistic to tell your children not to feel sad or upset if they are picked on or teased. It can be very painful to be called a name or shamed in front of others. It is important to empower your child with the tools to deal with such a situation if it happens in the future. Acknowledge how hard it is to ignore the person who hurts your feelings.
8. Try to alleviate tense social situations with humor. At home, laugh with your child about silly things and even about difficult things. Set an example for your child by not taking everything too seriously yourself. Also help your child improve self-soothing techniques. For example, teach your child to take deep breaths or count to ten before responding to others.
9. If your child has difficulty talking to you about problems at school, offer to have your child speak with another family member or, if necessary, a mental health professional. Talking about the hurt may alleviate the emotional pain your child experiences.
Recommended Reading List
American Academy of Child and Adolescent Psychiatry. Facts for Families. www.aacap.org.
The Facts for Families section provides information about wellness, preventing mental health problems,
disorders, and many related topics.
Brooks, R. and Goldstein, S. Raising Resilient Children: Fostering Strength, Hope and Optimism in Your
Child. Lincolnwood, IL: Contemporary Books, 2001.
Charkins, H. Children with Facial Differences: A Parent’s Guide. Bethesda, MD: Woodbine House, 1996.
Goldman, L. Raising Our Children to Be Resilient: A Guide to Helping Children Cope with Trauma in Today’s
World. New York, NY: Brunner-Routledge, 2005.
Huegel, K. and Verdick, E. Young People with Chronic Illness: True Stories, Help and Hope. Minneapolis, MN:
Free Spirit Publishing, 1998.
Kriegsman, K. Taking Charge: Teenagers Talk About Life and Physical Disabilities. Rockville, MD: Woodbine
House, 1992.
Lavin, Judith L. Special Kids Need Special Parents: A Resource for Parents of Children with Special Needs.
New York, NY: Berkley Books, 2001.
myFace. Parenting: A Guide for Parents of Children with Facial Differences. New York, NY: 2008.
For a copy of this publication, contact myFace: 333 East 30th Street, Lobby Unit, New York, NY 10016.
(212) 263-6656. www.nffr.org.
Operation Respect. Don’t Laugh At Me. For more information, contact Operation Respect: 2 Penn Plaza,
6th Floor, New York, NY 10121. (212) 904-5234. www.dontlaugh.org, email: info@operationrespect.org
Parr, T. It’s Okay to be Different. Singapore: Todd Parr, 2001.
Partridge, J. Arranging Faces: The Challenge of Facial Disfigurements. London: Penguin, 1990.
Seligman, M.E.P. Learned Optimism. New York, NY: Pocket Books, 1990.
Seligman, M.E.P., Reivich, K. Jaycox, L. and Gillham, J. The Optimistic Child. New York, NY: Houghton Mifflin,
1995.
In This Article
Click to jump to your selected section.