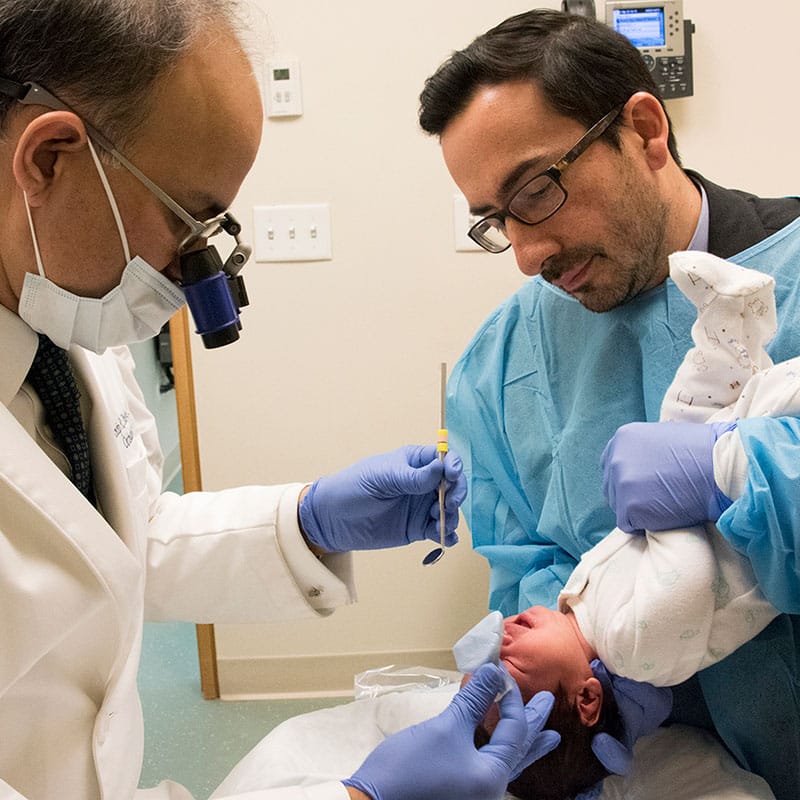
Nutrition
To download these guides in a PDF, click below:
A Guide to Children’s Nutrition for Parents of Children with Craniofacial Conditions
In This Article
Click to jump to your selected section.
Getting a Nutrition Evaluation
Nutrition Overview
Age-Specific Nutrition
Nutrition Considerations for Craniofacial Surgery
Tips for High-Calorie, High-Protein Nutrition Therapy
Managing Your Child’s Weight and Childhood Obesity
Nutrition with a Feeding Tube
Additional Resources
The purpose of this guide is to help patients with craniofacial conditions access information and resources to support optimal nutrition. Achieving and maintaining good nutrition is the foundation for a healthy life. This guide is meant to supplement the information provided by your/your child’s health care team and to provide a starting point from which to explore a nutrition plan for your child and family.
Good nutrition is important to everyone’s health, but even more important for individuals with specific health care needs such as those with facial conditions. Nutrition concerns vary depending on the type of facial condition. Many children with facial conditions experience trouble feeding, gaining weight, maintaining weight, and maintaining overall good nutrition. Because each and every child is different and may experience different nutrition issues, it is important to get an individualized nutrition assessment to determine the type of nutrition care plan that is needed.
Getting a Nutrition Evaluation
A nutrition evaluation is important if your child is having difficulties feeding, gaining weight, maintaining weight or is gaining weight too quickly. A nutrition evaluation is a comprehensive assessment conducted by the Registered Dietitian (RD).
The RD’s nutrition evaluation will involve assessment and monitoring of growth, caloric intake, nutrient intake, and fluid intake. In addition to an evaluation, the RD will provide nutrition counseling. The RD will give you recommendations for how much and what type of foods you/your child should be eating, how much fluid you/they should be drinking and approximately at what rate you/they should be growing. Everyone’s nutrition needs and concerns are different, and the nutrition assessment is designed to provide you with an individualized nutrition treatment plan to meet your/your child’s needs.
In addition to meeting with your healthcare treatment team, you/your child will meet with the dietitian for a nutrition evaluation before surgery or for any other reason deemed necessary by the healthcare team. This is an important step in the treatment process. Good nutrition status prior to surgery and throughout treatment will help with healing, recovery, and overall good health outcomes.
Nutrition Overview
Nutrition needs vary by age group and change yearly as a child grows into an adult. In general, everyone needs a good mix of all food groups. Balancing your diet to make sure you include all food groups is the best way to maximize nutrient intake. The following overview is a quick reference for food groups and appropriate portions of each. Carbohydrates, fats, and proteins provide us with calories and are considered macronutrients (meaning they make up the majority of our diet). Vitamins and minerals (such as calcium, vitamin D, and iron) help the body function efficiently – but don’t provide us with energy – and are considered micronutrients.
Carbohydrates
Carbohydrates (carbs) are any food that can be broken down by the body into sugar. The typical Western diet is mostly carbohydrates (~45-50% of daily calories). Since carbohydrates make up the majority of our calorie intake it is important to choose healthy carbohydrates more often. The trick to keeping your carbohydrate intake healthy is to choose mostly whole grain, high fiber complex carbohydrates (such as whole wheat bread, whole grain pasta, and brown rice) instead of simple sugars (such as candy, sweets, baked goods and white flours).
Carbohydrates include:
- Starches
- Sugars
- Breads
- Cereals
- Grains
- Baked goods
- Fruits
- Vegetables
- Beans and legumes
Proteins
Proteins are any food that can be broken down in the body to make amino acids. Our body requires protein for many things. Our muscles, hair, nails and skin are just a few parts of the body made from proteins. Protein makes up about 15-20% of our daily calorie intake.
Main dietary proteins include:
- Meat
- Fish
- Poultry
- Cheese
- Eggs
- Dairy
- Beans and legumes
- Soy
Fats
Fat is the highest calorie nutrient. We store fat on our bodies when there are more calories coming into the body than are going out of the body. For this reason, fat can be helpful for those who are trying to gain weight, but can be trouble for those who are trying to maintain or reduce weight. A small amount of fat is healthy (about 25-30% of daily calories). Choosing mostly healthy fats (such as unsaturated fats like olive oil, canola oil, nuts/nut oils, seeds/seed oils, fish oils) instead of unhealthy fats (saturated and trans fats such as butter, animal fats and hydrogenated oils) can help with heart health and overall health.
Unsaturated and saturated fats include:
- Oils
- Butter
- Animal fats (lard)
- Mayonnaise
- Cream
- Nuts and seeds
Keeping a balance of all these nutrients is key. Excluding a whole food group is not recommended unless directed by your doctor or dietitian for a specific reason. Each meal should contain a balance of carbohydrates, fats and proteins. Think of dividing your plate into sections.
VIDEO: Sandi Aubuchon, President of Dr. Brown’s Medical discusses nutrition for kids with cleft and craniofacial conditions
Age-Specific Nutrition
Nutrition for Infants (0-1 Years)

The nutrition needs of the infant are aimed at promoting and maintaining good growth and weight gain. Calorie and protein needs are high during the first year of life. As the infant grows, nutrition needs as well as food sources change.
For the first year of life breast milk or an iron-fortified infant formula will be the main source of nutrition. Any milk not specifically designed for infants (cow’s milk, goat milk, rice milk, or soy milk) is not recommended before the 12-month mark. Breast milk has many nutrition and health benefits and is considered the best food for your baby. If you are unable to/choose not to breastfeed or if your child is having difficulty breastfeeding, commercial infant formulas are available and provide similar nutrition to human breast milk.
Frequency of feeding depends on the age of the baby. Younger infants take less formula per feeding and need to be fed more often than older infants. You will know your infant is getting enough to eat if they are growing and gaining weight, which makes tracking their growth and weight gain very important. In the first days of life infants will lose weight, but within 2 weeks they should regain their birth weight. In general, it is recommended that a baby doubles their birth weight by 4-6 months and triples their birth weight by 12 months of age. Below is a chart of typical infant feeding, type of nutrition as well as typical growth rates. In general, frequency of feeding should be based on the infant’s signs of hunger and satiety. The type of nutrition will vary depending on the developmental readiness of the baby, but the following chart can help you get an idea of feeding and growing trends for the typical infant.
Typical Intake for Infants
1-4 MONTHS
-
- Infant formula or breast milk (2-4 ounces per feed)
- 8-12 feedings per day
- Expected 25-30 grams per day weight gain (NOTE: approximately 28 grams is equal to 1 ounce)
4-6 MONTHS
-
- Breast milk or infant formula (typically 6-8 ounces at each feed, 4-6 feedings per day)
- Infant cereal (1-2 tablespoons each feed, 2-3 times per day). At age 6 months you can begin to incorporate solids in the form of infant cereals. Solids should only be introduced if your baby is showing signs of readiness (holding their head up, interested in the spoon, etc.). Infant cereal should be fed to the baby with a spoon and should not go into the bottle unless directed by your dietitian or healthcare team.
- Expected 15-20 grams per day weight gain
6-8 MONTHS
- Breast milk or infant formula (typically 6-8 ounces at each feed, 3-5 feedings per day)
- Infant cereal (2-4 tablespoons, 2 times per day)
- Baby foods (fruits and vegetables, proteins) and homemade purees. At 6 months your baby may be more interested in baby foods. If they are able to hold their head up and be fed with a spoon, you can start giving them baby foods. There are three stages of baby food purees (stage 1, 2 and 3) before your baby will eat solid table foods. Start with stage 1 baby foods and progress from there depending on your baby’s tolerance.
- Expected 10-13 grams per day weight gain
8-12 MONTHS
- Breast milk or infant formula (typically 6-8 ounces, 3-4 feedings per day). Your baby will still be using formula or breast milk until approximately age 12 months. As they move towards the 12-month mark formula intake will taper off as solid food intake increases. At 1 year you can incorporate whole cow’s milk.
- Baby foods. Food will begin taking the place of formula or breast milk as the baby grows. Typically, babies will still feed 4-5 times per day, but there will be a mix of baby foods and formulas. Dairy such as baby yogurt or cheese can also be introduced at this age. High iron foods such as beans or meat are important at this stage as the main source of iron (formula or breast milk) is being tapered off.
- Eggs are introduced. Ask your pediatrician, but new recommendations are to give the entire egg and not worry about allergies.
- Experiment with finger-foods! Some examples are low sugar cereal (Cheerios®), small chunks of banana or avocado, small pieces of soft cheese, chopped hard-boiled egg, pea-sized pieces of cooked soft meats (chicken, meatballs, etc.).
- Expected 10-13 grams per day weight gain
You will know your baby is getting enough nutrition if they are growing, gaining weight and appear happy and content. Crying, retching, stopping after an ounce, arching their back away from the bottle, waving arms and vomiting after meals could be a sign that your baby is not digesting their food well. This could also be a sign of reflux, which is a common problem in young infants. Reflux refers to a condition where the contents of the stomach are spit out shortly after feeding. Reflux can only be diagnosed by the doctor and usually gets better as the infant grows. If your baby is vomiting often, crying or appears uncomfortable during/after feeding, speak with your primary healthcare provider. Special infant formulas and feeding techniques can be recommended to help with reflux and feeding intolerance so that your baby can get enough nutrition comfortably. For children with a cleft palate, medication is often required to manage reflux with or without spit up.
Feeding Considerations for Infants with Cleft Lip/Palate
Because of the inability to create suction, infants with cleft lip/palate may have difficulty feeding from the breast or a standard bottle and will likely require adaptive feeding equipment. If your infant is having trouble feeding, you and your cleft team can come up with a solution to effectively feed your baby. The cleft team can help you select adaptive feeding equipment (such as special bottles, nipples and valves) and helpful positioning to successfully feed your infant. For more information on feeding an infant with cleft lip/ palate, the American Cleft Craniofacial Association (ACPA) has a very informative feeding video entitled “Feeding Your Baby.”
Nutrition for Toddlers (Ages 1-3 Years)

By one year of age your baby may be ready to advance to table foods. As they advance to solid foods it is important to minimize choking risk. The following foods should be avoided as they increase choking risk in infants:
- Popcorn
- Peanuts
- Raisins, whole grapes
- Uncut, stringy meats
- Hot dog pieces
- Hard, raw fruits or vegetables such as apples, green beans
- Sticky foods such as peanut butter, which can get stuck in the back of mouth
- Any other pieces of food that the infant cannot chew because he or she does not have advanced chewing skills yet. Un-chewed food can block the airway, because babies cannot cough and clear their throats on their own.
During this time children are also learning to be independent with feeding. Encouraging self-feeding and providing nutrient-rich foods is the role of the caregiver. Children of this age can meet all of the recommended intakes for vitamins and minerals with a varied diet. Therefore, introducing your toddler to new and exciting foods is key to maximizing nutrient intake. It is at this age that a child will begin to sort their likes and dislikes. Promote vegetables, meats and cow’s milk to ensure your toddler’s iron and calcium needs are being met.
Nutrients of Concern: Calcium & Iron
The recommended calcium intake for this age group is 700 milligrams per day. To maximize calcium intake, encourage cow’s milk. (NOTE: whole cow’s milk should be used up until 2 years of age. After age 2 your toddler needs less fat and whole milk should be switched out for 1% or skim milk). If your child is lactose intolerant or dislikes cow’s milk, incorporate foods fortified with calcium (soy milk, almond milk, calcium-enriched orange juice, cheese, or other culturally appropriate foods high in calcium). Refer to the list of high calcium foods in Appendix A to help increase calcium intake in your child’s diet. The recommended intake of iron for this age group is 7 milligrams per day. To make sure your toddler is getting enough iron check the list in Appendix B for high iron foods and tips on getting more iron.
Nutrition for Preschool-Aged Children (Ages 4-5 Years)

Children ages 4-5 years may be feeding in several different environments during the day, making it difficult to properly assess calorie and nutrition intake. Your child’s preferences are developing during this time. Although it is great that your child is beginning to make their own decisions, this can make meal times stressful for caregivers with “picky” eaters. To avoid power struggles and control issues, caregivers should know that they are only responsible for what the child is offered to eat and where and when it is presented. The child is then responsible for how much food he or she eats.
Here are some tips to help the caregiver manage meal times for the preschool child.
- Provide a quiet, distraction-free environment for meals and snacks. Avoid television or radio.
- Allow the child to decide how much or even whether or not to eat from 2 or 3 healthful food choices provided. An occasional skipped meal is not cause for concern because children usually make up their intake at subsequent meals or over the course of days. Do not bribe or force the child to clean his or her plate, as this may lead to overeating or development of an aversion to foods.
- Encourage at least one bite of a new food. It may take many introductions of the food before they will try it. Try not to trick, bribe, or force a new food.
- Involve the child in meal and menu planning, offering 2-3 choices. Serve the child most of the same food that the family is eating to avoid making separate meals for everyone.
- Employ a sous-chef (as in your preschooler)! Get your child involved in meal planning by asking them help prepare some of the food. For example, at this age asking your child to tear the lettuce for your dinner salad. Getting them involved will pique their interest at meal times.
- Keep desserts and sweets as the usual last course of meals. Try not to use desserts and sweets as a reward for finishing a meal. Studies have shown that this can teach the child that dessert is the best part of the meal and may increase the child’s preference for sweet foods.
Nutrients of Concern: Calcium & Iron
Calcium and iron remain important nutrients throughout growth. Calcium needs increase to 1000 milligrams per day and iron needs increase to 10 milligrams per day. Trying new foods and keeping the diet varied to maximize nutrient intake is extremely important in this age group. This is the time during which food preferences and lifelong eating patterns are solidified. The more varied the diet, the more nutrients the child will consume.
Nutrition for School-Aged Children (Ages 5-11 Years)

Nutrition for school aged children focuses mainly on avoiding serious health concerns such as iron- deficiency anemia, undernutrition, obesity, eating disorders, and dental caries. Nutrition is also focused on promoting lifelong behaviors to reduce the risk for chronic diseases of adulthood such as heart disease, diabetes, high blood pressure, some forms of cancer, and osteoporosis. Your child should still be growing and gaining weight at an appropriate rate (approximately 4-6 pounds per year and 2-3 inches per year).
Another concern in this age group is food allergies. Having multiple food allergies can place a child at risk for several nutrient deficiencies and slow growth. If your child has been diagnosed with a food allergy, it is recommended that your child be seen by our team, including the RD, to help you replace nutrients in the diet that might be lost with the elimination of a food or food groups.
Nutrients of concern in this age group emerge because of the replacement of nutritious foods with foods of lower nutrient content. For example, low calcium intake may be related to replacement of milk by fruit juice and soft drink consumption. Unhealthy foods are all around your children now (in school, on TV, in the grocery store) so it is important to help guide them towards nutritious foods.
Nutrients of Concern: Calcium, Vitamin D and Iron
Calcium, vitamin D, and iron are the most important nutrients for this age group.
Calcium — Calcium intake has been reported to be low in school aged children. Calcium needs increase to 1300 milligrams per day. Children that are unable to consume adequate amounts of calcium rich food should speak with their doctor about supplementation. Find the calcium content of different foods here.
Vitamin D — High rates of vitamin D deficiency have also been noticed in this age group. The best way to get dietary vitamin D is to eat foods that have been fortified with the vitamin (fortified dairy products, fortified cereals and juices and fatty fish). It is important to remember that calcium cannot be absorbed without vitamin D. Fortified dairy is the best way to get dietary vitamin D. The current recommendation is to provide vitamin D supplementation to all children and adolescents who do not receive >200 IU/day of fortified foods.
Iron — Iron is still important, but the recommended daily intake drops to 8 milligrams per day for children of this age. Find the iron content of different foods here.
The biggest health concern for children this age is overweight and obesity. In the past 30 years the rates of obesity and type 2 diabetes have significantly increased in this age group. Low activity levels and excess calorie intake contribute to weight gain. If your child is overweight or gaining weight too quickly, speak with the dietitian to help get them design a healthy weight loss plan. Weight loss can be tricky at this age because the goal is to slow or stop weight gain while encouraging linear growth (height) to make sure overall growth does not become stunted. For this reason, it is best to consult the dietitian for an individualized plan to get the correct calorie and exercise goals for your child. However, everyone can make subtle changes to improve their nutrition intake. It is never too early or too late to begin making healthy changes. Please refer to the section on managing overweight and obesity for some quick dietary tips.
Nutrition for Adolescents

With the arrival of puberty there is a significant increase in physical growth and development, resulting in greater nutrition needs. Growth rates increase during puberty, with females averaging 3-4 inches per year and males averaging 3.5-4.5 inches per year. Weight gain should remain relatively stable at 4-6 pounds per year. This opportunity for increased linear growth helps some adolescents “thin out” by becoming taller and leaner while maintaining the same rate of weight gain.
Adolescence is a key time for establishing healthful eating behaviors that promote maintenance of a healthy weight. Solidifying sound eating habits can prevent chronic diseases including; diabetes, high cholesterol, and heart disease. Calorie and protein needs nearly double during adolescence, but as these needs increase, it is important to balance calorie intake with exercise to avoid excess weight gain. On the other end of the spectrum, eating disorders may develop. Increased societal and peer pressure to be thin can cause adolescents to develop unhealthy eating practices such as severe food restrictions, binging or purging. Eating disorders are a very serious health concern. If you suspect your child has an eating disorder, talk to them about healthy eating and healthy body image. Then consult with a school counselor and your health care team immediately.
Nutrients of Concern: Calcium, Vitamin D and Iron
With the arrival of menstruation in women, iron becomes more important. Calcium remains important as bones continue to grow in length and width. There is no “set” age for when adolescents stop growing in height, but height growth usually stops between the ages of 16-18 years in females and 18-22 years in males. The cessation of linear growth in males and females is often the determination for the timing of jaw surgery in patients with craniofacial conditions. Linear growth usually stops 1-4 years after puberty, but bones continue to grow in width until age 25-28. Calcium and vitamin D remain critical nutrients throughout this time and throughout life. Calcium needs remain high at 1300 milligrams per day. Iron needs increase to 15 milligrams for females and 11 milligrams for males.
Nutrition Considerations for Craniofacial Surgery
Individuals with craniofacial conditions (including cleft lip/palate) often undergo multiple surgical procedures. Feeding is often disrupted because of the nature and location of these surgeries and can lead to post-surgical weight loss. The best thing you can do to prepare you/your child for a speedy recovery is to be well-nourished prior to surgery. A nutrition evaluation will take place before craniofacial surgery. It is at this time that the dietitian will review how many calories, how much protein, how much fluid you/your child should be consuming. Calorie needs are increased after surgery, so knowing your recommended daily intake is important for creating appropriate meal plans.
Pre-Surgical Nutrition Optimization
Making sure you or your child is well nourished before surgery is extremely important. Getting enough calories and protein should be a focus for parents and patients prior to any surgery. If you or your child has experienced weight loss or poor intake, an evaluation by an RD would be needed to make sure nutrition status is optimal prior to surgery. The dietitian will help tailor a nutrition plan to help prepare you for the surgery and healing process
Post-Surgical Nutrition Concerns
Eating after surgery can be painful, tiresome and difficult for many patients who have had cleft lip/palate or craniofacial surgery and makes obtaining adequate nutrition after surgery challenging. In addition, calorie and protein needs are increased post-surgically to help with healing and recovery. Calorie and protein needs can increase to one and a half times those of pre-surgery. The diet progression after surgery is usually gradual, advancing from liquids to pureed foods to soft solids as the patient can tolerate it. Liquid or pureed foods may have less calories and protein than traditional solids; therefore, it is important to take extra steps to maximize the calories and protein in each meal. Making sure your or your child’s diet is high enough in calories and protein is an important component of the healing process.
After surgery, patients will likely experience something called “dysphagia,” which refers to difficulty swallowing or difficulty chewing. An alternative textured diet (such as the ones listed below) may be required until you or your child is fully healed. It may be easier to eat foods that are pureed, liquefied or can be mashed with a fork. These textures require less chewing than traditional solids, making them easier to eat.
The diets listed below are typical following surgery. Your healthcare team will advise as to how long you or your child needs to be on a particular diet. If you are scheduled to be on one of the following diets for longer than three days, the dietitian can help you create a high calorie/high protein meal plan that is nutritionally complete while maintaining the appropriate texture.
Clear Liquid Diet
This diet includes liquids that are clear at room temperature.
- Foods allowed on this diet include juice, ice water, popsicles, ice chips, sweetened tea or coffee, soda, meat or vegetable broths.
- This diet is not nutritionally adequate and typically lasts 24-48 hours.
- If you or your child will be on this diet for longer than 3 days, speak with the dietitian or healthcare team about starting a nutrition supplement (a high calorie, high protein drink that is allowed on the clear liquid diet).
Full Liquid Diet
The full liquid diet allows all liquids as well as thin cereals and soups.
- Foods allowed on this diet include all liquids allowed on the clear liquid diet with the addition of milk, thin cereal (oatmeal, cream of wheat), strained cream soups, milkshakes, custard, puddings, juices or nectars that contain pulp, and melted ice cream.
- This diet can be nutritionally complete if high calorie, high protein foods are included in the meal plan. If you or your child will be on this diet for longer than 3-5 days speak with your dietitian about starting a nutrition drink or shake to help increase calorie, protein and vitamin/mineral intake.
Puree Diet
This diet includes foods that can be safely and easily swallowed.
- Foods allowed on this diet include all foods that are whipped, mashed or blended until they are a “pudding” like texture. Coarse textured foods such as raw fruits and vegetables should be avoided unless they are completely pulverized in a blender.
- All foods should be smooth and free of lumps.
- The puree diet is nutritionally complete and can be high calorie, high protein depending on the foods incorporated into the meal plan. It can be challenging to get your recommended protein intake on a puree diet because pureed proteins are generally not as well-accepted as other purees. Speak with your dietitian about making the puree diet high in both calories and protein to maximize healing.
- Here are some additional tips for making the puree diet high calorie/high protein.
- Mix in shredded or melted cheese
- Mash beans into a puree
- Add milk or yogurt to purees
- Cooked egg yolks can be easily pureed and are well accepted
- If your child will not accept any of the above methods, you can talk to your dietitian about adding a protein powder to meals (1 packet or scoop usually has as much protein as an egg)
- Add small amounts of gravy, sauce, half and half, heavy cream, vegetable juice or milk
- Add potato flakes or commercial thickeners if purees are too thin. This will also add calories
- Add dry milk powder to purees to increase calories, protein and thickness
- Also see the section on “High Calorie, High Protein Nutrition Therapy” for more tips
Soft/Mashable Diet
This diet includes foods that are soft and can be safely and easily swallowed.
- Foods allowed on this diet include all foods that are soft and easy to swallow, foods that can be easily “mashed” with a fork and nearly all regular foods EXCEPT sticky, hard or crunchy foods.
- This diet is nutritionally complete as it includes all regular textured foods. Cook foods until tender and make sure they can be easily mashed with a fork for swallowing ease
Tips for High-Calorie, High-Protein Nutrition Therapy
Patients undergoing craniofacial surgery need high protein, high calorie nutrition therapy for optimal healing. In addition, those who are underweight or growing slower than average will also require high calorie, high protein nutrition therapy. Speak with the dietitian about starting a high calorie, high protein nutrition plan. Below are some tips to help you get started!
Tips for Adding Calories
- Avoid “light” or “diet foods” which are usually low in calories. (See the table for a list of high calorie foods.)
- Add heart healthy oils to meals or snacks (olive oil, flax oil, nut oils). Each tablespoon is equal to 120 calories.
- Sprinkle cheese into veggies or starches. Each ounce of cheese is around 100 calories.
- Add heavy cream to smoothies. Each tablespoon is 50 calories.
- Make high calorie, high protein recipes.
- Eat at least 4 small meals and 2 snacks daily. Eating more frequently can help increase calorie content throughout the day.
- Add fat to meals. Each tablespoon is roughly 100 calories. Fat is the most calorie dense nutrient, making it an easy way to add calories in a small dose! Some examples of fat are butter, oils, cream, mayonnaise, margarine, peanut butter, nuts and nut butter, full fat dairy, avocado.
- Drink healthy beverages that add calories. For ex- ample, have fruit or vegetable juices/nectars, milk, or shakes. If needed, drink a nutritional supplement to help reach calorie goals. (NOTE: nutritional supplements should not be used as meal replacements unless instructed by your healthcare team. These drinks are meant to supplement (meaning add to) your/your child’s calorie intake, not replace foods or meals).
- Choose cooking methods that use added fats and oils, such as frying or sautéing.
- Some children eat more if they can help plan, shop for and prepare meals. Include your child if it will help him/her eat more.
Tips for Adding Protein
- To get more protein include a protein serving at each meal. (See the table for a list of high protein foods.)
- If high protein items are not an option because of preferences or textural restrictions, speak with your dietitian about adding protein powder (a tasteless powder concentrated with protein) to meals to meet protein needs
Managing Your Child’s Weight and Childhood Obesity
Childhood obesity is becoming an increasing national health crisis. With nearly 30% of children classified as overweight or obese, our nation is facing an epidemic. It is important that your child learn healthy eating habits at an early age to facilitate lifelong healthy eating practices. All children should be introduced to healthy foods and be educated on proper nutrition, but if your child has been classified as overweight/obese or if they have been gaining weight at a rapid rate, it may be time to adopt a nutrition plan that will help slow down or reverse excess weight gain. Weight management involves changing what you eat and how you move. Eating more calories than you burn in a day is how you gain weight. Therefore, if you need to lose weight, it is important that you cut back on your calorie intake by reducing portion sizes or changing the types of food you eat to low calorie foods and/or increase the amount of energy you burn in a day by exercising.
Tips for Weight Loss
- Cut back on portion sizes. Smaller portions are those that take up 1/3 or less of a plate. A large portion would take up 1/2 or more of a plate.
- Avoid sugar sweetened beverages such as sodas, iced teas, lemonades, juices and sports drinks. These drinks are packed with calories and sugar and have very little nutritive value. Drink water, seltzer, un- sweetened teas and low-fat dairy instead.
- Eat at least 3 meals and 1-2 snacks per day to avoid “grazing” throughout the day or over-eating at a meal.
- Eat plenty of vegetables! Veggies are low in calories and are packed with nutrition and fiber. 1 cup of broccoli is only 40 calories compared to one cup of pasta or rice which is 180 calories.
- Stick to lean protein such as fish and lean meats. Meats labeled “loin” or “round” are leaner. Always cut away visible fat from meats and remove skin from chicken and other poultry.
- Choose low fat dairy (1% or skim milk and low-fat cheeses and yogurts).
- Read labels and scrutinize products! Always compare products to find the lowest calorie options.
- Get plenty of fiber. Vegetables, fruits, and whole grains are good sources.
- Plan meals ahead of time.
- Choose healthy cooking methods such as baking, broiling, sautéing, grilling and steaming. Avoid deep frying. When cooking with oils, limit to 1 tablespoon – use non-stick cooking spray and low sodium broths if needed.
- Use smaller plates, bowls, glasses and serving spoons.
- Divide your plate into four equal parts. Use one part for meat, one for starch (such as pasta, rice, potatoes, or bread) and two for non-starchy vegetables. (Starchy vegetables include carrots, corn, peas, plantains, potatoes, yams, yucca, etc.).
- Snack smart! Choose snacks that contain less than 10 grams of sugar, at least 2 grams of fiber and less than 2 grams of saturated fat per serving.
- Get active: exercise as tolerated. Everyone should get at least 60 minutes of exercise daily. Make exercise a family affair and play a game or make up a dance to get the whole family moving.
Managing Nutrition with a Feeding Tube
Some patients may require a feeding tube to meet their nutrition needs either while they are learning to safely consume a diet by mouth or while they are unable to meet their nutrition needs by mouth alone. Guidelines for type and amount of tube feeding will be prescribed by the health care team and monitored by the RD. If you or your child will be maintained on a tube feeding regimen, make sure to meet with the dietitian regularly to make sure you/they are getting enough calories, protein, fluid and a nutritionally appropriate formula. The following resources may be helpful if you would like more information about tube feedings:
Additional Resources for Parents and Patients
In addition to the information in this guide, you can use these credible and informative resources to get more information.
- Academy of Nutrition and Dietetics. http://www.eatright.org/
- The United States Department of Agriculture, Choose My Plate. http://www.choosemyplate.gov/
- Information on vitamins and minerals. Oregon State University, Linus Pauling Institute, Micronutrient Information Center. http://lpi.oregonstate.edu/infocenter/
Appendix A: Calcium Content of Foods List
|
CALCIUM PER SERVING |
FOOD |
|---|---|
| High Calcium (300 mg per serving) |
|
| High Calcium (200 mg per serving) |
|
| Moderate Calcium (150 mg per serving) |
|
| Moderate Calcium (100 mg per serving) |
|
| Moderate Calcium (50 mg per serving) |
|
With permission from Academy of Nutrition and Dietetics, Nutrition Care Manual® (NCM) © 2012 http://nutritioncaremanual.org. Accessed March 25, 2013.
Appendix B: Iron Content of Foods List
| IRON PER SERVING | FOOD | AMOUNT (MG) |
|---|---|---|
| High Iron (at 2 mg per serving) | Beef or veal (3 ounces) | 3 |
| Clams, oysters, shrimp, sardines (3 ounces) | 3 | |
| Bran flakes (1/2 cup) | 18 | |
| Cream of wheat (1/2 cup) | 5 | |
| 100% Iron fortified cereal | 18 | |
| Oatmeal fortified (1/2 cup) | 5 | |
| Baked potato with skin (1) | 3 | |
| Dried beans (1/2 cup; lima, lentils, navy and kidney) | 2.5 | |
| Soybeans (1/2 cup) | 4 | |
| Tofu (1/2 cup) | 3 | |
| Spinach (1 cup) | 3 | |
| Moderate Iron (1 – 2 mg per serving) | Poultry (3 ounces) | 1 |
| Corned beef (3 ounces) | 2 | |
| Cooked kale (1 cup) | 1 | |
| Dried apricots (7 halves) | 2 | |
| Raisins (5 tablespoons) | 1 | |
| Whole wheat bread (1 slice) | 1 | |
| Nuts (1 ounce; cashews, brazil nuts, walnuts) | 1 |
Reprinted with permission from Academy of Nutrition and Dietetics, Nutrition Care Manual® (NCM) © 2012 http://nutritioncaremanual.org. Accessed March 25, 2013.
In This Article
Click to jump to your selected section.