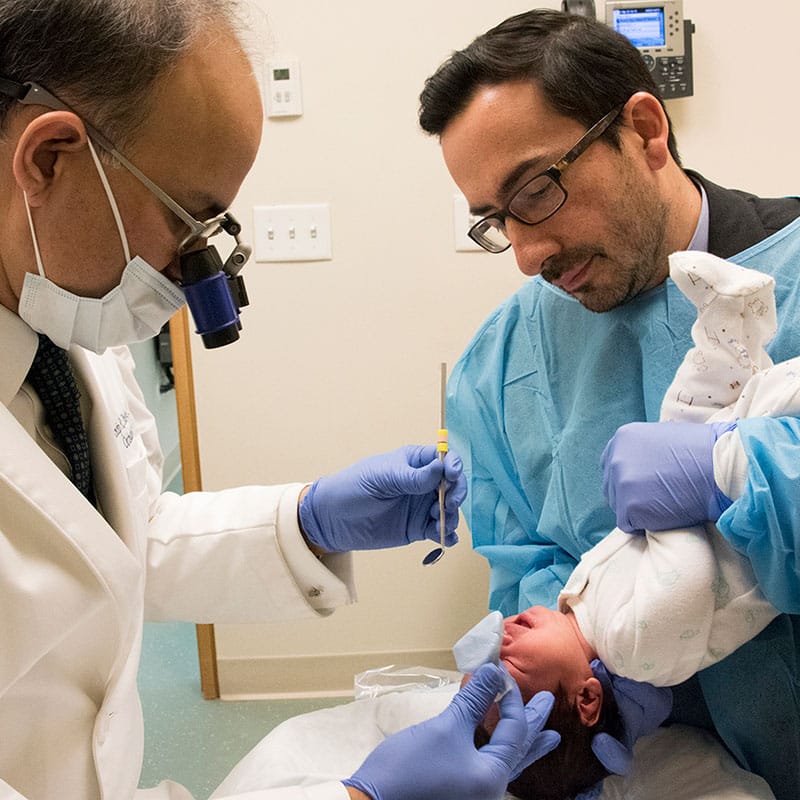
Craniofacial Microsomia (Including Hemifacial Microsomia and Goldenhar Syndrome)
In This Article
Click to jump to your selected section.
What is Craniofacial Microsomia?
Prevalence
Causes
Signs & Symptoms
Diagnosing
Treatments & Procedures
Living with Craniofacial Microsomia
Potential Complications and Challenges
Meet a Member of the myFace Community
myFace Direct Services and Educational Programs
Resources for the Craniofacial Community
Home > Craniofacial Conditions > Craniofacial Microsomia
Learn About Craniofacial Microsomia
Craniofacial microsomia (CFM) is the second most common birth defect that affects the face after cleft lip and palate. In patients with craniofacial microsomia, part of the face appears smaller than normal, and often other structures – including the eyes, ears, cheek and jaw bones – are also affected.
What is Craniofacial Microsomia?
Although there is no definitive consensus among experts, it is thought that craniofacial microsomia represents a spectrum of conditions, and the features can occur in variable combinations and can range from very mild to severe.
Craniofacial microsomia is also sometimes referred to as first and second branchial arch syndrome or oculo-aural-vertebral syndrome.
Hemifacial microsomia
In 85-90% of cases, only one side of the face is affected – most commonly the right side. This is often referred to as hemifacial microsomia, a condition that results in one side of the face being smaller or underdeveloped relative to the other side, resulting in facial asymmetry. Hemifacial microsomia typically affects the ear, mouth, and jaw. Sometimes, structures such as an ear or jaw bones, may be missing. Typically, only the lower part of the face is affected. However, the eye and forehead may also be affected in more severe cases.
Hemifacial microsomia impacts the bone, muscle, fat and nerves of the face. Some of the characteristics of hemifacial microsomia include: shortened jaw set at an angle on the affected side, angled chin, altered positioning of teeth (dental malocclusion), cleft lip/palate or oral lateral cleft lip, reduced soft tissues in cheek, small or missing ear, skin tags on the cheek or near the ear, and absence or dysfunction of facial nerves on the affected side. Some babies born with hemifacial microsomia have minor facial changes, while others have more severe changes. This condition is progressive as the affected side of the face does not grow at the same rate as the unaffected side of the face.
Goldenhar syndrome
Goldenhar syndrome is very similar to hemifacial microsomia and can be considered a variant of hemifacial microsomia that includes some additional characteristics, such as vertebral anomalies, heart and kidney defects, benign growths on the eye called epibulbar dermoids, narrowing of one eye, and notched eyelids. People with Goldenhar Syndrome are more likely to have both sides of the face affected. They are also more likely to have more severe facial alterations, including more severe jaw and soft tissue changes, and a higher incidence of macrostomia. Macrostomia is a form of a facial cleft; due to the failure of embryonic structures of the face to form properly, the result is an enlargement of the mouth.
In summary, while there is inconsistency in the naming and classification of craniofacial microsomia, hemifacial microsomia, and Goldenhar syndrome across the literature, it is likely that they are all part of a spectrum of related conditions. In general, hemifacial microsomia refers to the asymmetrical growth of the face, while craniofacial microsomia has additional cranial anomalies. Finally, patients with Goldenhar syndrome have the features of craniofacial microsomia and/or hemifacial microsomia, and additionally are likely to have vertebral malformations, epibulbar dermoids, as well as heart and kidney defects.
Prevalence of Craniofacial Microsomia
Craniofacial microsomia is the second most common craniofacial condition after cleft lip and palate, affecting 1 in every 3,000 to 5,000 live births. It occurs more often in males than in females. Since Goldenhar syndrome is likely a variation of craniofacial microsomia and hemifacial microsomia, it is more rarely reported; the incidence of Goldenhar syndrome has been reported as a wide range, from 1 in 3,500 to 1 in 26,5500 births. However, the most commonly accepted estimate is about 1 in 5,600 births. Similar to craniofacial microsomia and hemifacial microsomia, Goldenhar syndrome appears to be slightly more common in male babies compared to female babies.
What are the Causes of Craniofacial Microsomia?
The exact cause of craniofacial microsomia and associated conditions such as Goldenhar syndrome and hemifacial microsomia remains unknown, but the clinical manifestations are thought to be the result of abnormal development of the first and second pharyngeal arches during the first 6 weeks of life.
More specifically, there may be an impairment in the movement of specialized cells (called neural crest cells) that migrate from the vicinity of the spinal cord to the developing face, where they form the facial skeleton during fetal development. If too few of these cells migrate to their intended destination, that side of the face may end up being smaller. There is also some evidence to suggest that compromised blood flow to the fetus’ developing face may contribute to this condition.
Genetic Basis of Craniofacial Microsomia
At this time, there is no specific gene that has been found to cause craniofacial microsomia, hemifacial microsomia, or Goldenhar syndrome on a consistent basis. Most cases of craniofacial microsomia are actually sporadically acquired, which means there is no family history of the disease. In only about 2% of cases, children appear to inherit the condition from a parent in an autosomal dominant pattern; this means that children of an affected parent have a 50% chance of inheriting the condition.
Despite the largely unknown genetic basis of craniofacial microsomia, ongoing studies are beginning to identify mutations that are associated with the condition. One study found that a mutation in the SF3B2 gene (which produces a small cellular protein) was associated with both inherited and sporadic cases of craniofacial microsomia. It is thought that mutations in the SF3B2 gene may disrupt cranial neural crest cell development, resulting in craniofacial microsomia. To date, SF3B2 gene mutations are the most frequently observed genetic basis of craniofacial microsomia, but they still only account for 5% of cases. Other genes that have been implicated in the condition include MYT1, OTX2 and PLCD3. In autosomal dominant inherited cases, experts have also identified some regions in chromosomes 11 and 14 that appear to be involved, but the specific gene(s) responsible are not yet known.
Non-Genetic Basis of Craniofacial Microsomia
Some research studies have also suggested that some non-genetic factors, such as conditions during pregnancy and use of certain medications during pregnancy, can contribute to increased risk of craniofacial microsomia. These include:
- Diabetes during pregnancy
- Tobacco use (especially during the second trimester)
- Retinoic acid (such as isotretinoin or Accutane, which is often used as an acne medication)
- Being pregnant with more than 1 child
Signs & Symptoms of Craniofacial Microsomia
During fetal development, structures known as the first and second brachial arch will eventually develop into the head and neck. The abnormal development of these structures results in the distinctive facial features of craniofacial microsomia and related conditions. Most patients have facial asymmetry or hemifacial microsomia, where one side of the face appears different than the other. This is due to the underdevelopment of the jaw, cheekbones, and facial muscles. Of note, although hemifacial microsomia is the most common presentation, both sides of the face can be affected in up to 1 in 3 patients.
Learn more about signs & symptoms of Craniofacial Microsomia →
Diagnosing Craniofacial Microsomia
Unfortunately, there is no established set of diagnostic criteria for craniofacial microsomia or other associated conditions. The diagnosis is made based on observing the physical features of a child at birth. Since there is a wide range of physical presentations, from mild to severe, which affect different facial structures, clinicians have developed a classification system to distinguish various patterns of physical presentations. These classification systems help to guide treatment plans. The most widely used is the OMENS classification system (OMENS stands for orbit, mandible, ear, nerve, and soft tissue), with each feature given a severity score. This classification system helps in developing an optimal treatment plan.
It is rare that a prenatal ultrasound may be able to detect features of craniofacial microsomia, including abnormalities of the jaw, ear, or mouth.
After diagnosis, additional tests may be needed to further evaluate the nature and extent of the anomalies. These may include:
- CT scan – detects ear structure abnormalities that may put a child at risk for hearing loss
- Echocardiogram (ultrasound of the heart) or electrocardiogram (ECG) – evaluates the heart for structural or functional defects
- Eye exam – detects abnormalities of eye structure
- Hearing test – assesses the extent of any hearing loss
- X-rays – evaluate bone structure anomalies (e.g., skull, spine, ribs, and limbs)
- Ultrasounds – evaluate the structure of kidneys and other organs
- Sleep studies – evaluation for obstructive sleep apnea
- Pulmonary function tests – measure the lung’s ability to intake and expel air and efficiently oxygenate the body; this test helps diagnose thoracic insufficiency syndrome.
Since there is no specific gene or gene(s) that are consistently associated with craniofacial microsomia, hemifacial microsomia, or Goldenhar syndrome, genetic tests are not routinely used for diagnosis. Nevertheless, genetic testing may be recommended to rule out other genetic conditions that can cause similar signs and symptoms, such as Treacher Collins syndrome. Genetic counseling can also help families understand the potential risk of having another child with this condition.
Treatments & Procedures for Craniofacial Microsomia
The treatment of craniofacial microsomia varies based on the types and extent of anomalies. Children with mild symptoms may not need any treatment, while others with more severe symptoms will need to work with a team of specialists to create an individualized care plan to address each individual symptom and determine the timing of various interventions.
Read more about Treatments & Procedures for Craniofacial Microsomia →
Living with Craniofacial Microsomia
While most patients with craniofacial microsomia, hemifacial microsomia, Goldenhar syndrome, and other conditions in this spectrum are able to live a full life with normal life expectancy, they do often face the ongoing challenges of living with disabilities. Hearing and visual disabilities are the most common, and some patients may continue to need support for speech and swallowing issues. Also, about 15% of patients with Goldenhar syndrome may have an intellectual disability and may need more day-to-day living support.
The continued follow-up and monitoring of patients with craniofacial microsomia depends on the resulting conditions affecting each patient. Many patients are followed by a craniofacial team that includes specialists such as an otolaryngologist (ear, nose, and throat, or ENT, doctor), ophthalmologist (eye doctor), plastic surgeon, audiologist, neurologist and neurosurgeon, dentist or maxillofacial surgeon, and speech therapist.
For patients who have issues in other organ systems, additional long-term care may be needed from specialists such as:
- Orthopedic surgeons to treat spine or limb abnormalities
- Pulmonologists to monitor and treat lung and breathing conditions
- Cardiologists to treat and monitor heart defects
- Urologists to monitor and treat kidney and bladder conditions
Potential Complications Experienced by People Living with Craniofacial Microsomia, Hemifacial Microsomia, and Goldenhar Syndrome
Lastly, there can be social, emotional, and psychological challenges for children with craniofacial microsomia and associated conditions. Patients may feel worry or anxiety about their appearance and have trouble in social situations. In addition, children may feel extreme stress having to undergo multiple medical interventions. Thus, working with a psychologist or other mental health provider can be beneficial to help ensure social and emotional well-being for people living with this condition.
Meet a Member of the myFace Community
myFace Provides Support for People Living with Hemifacial Microsomia, Goldenhar Syndrome, and Other Craniofacial Conditions
myFace provides a variety of direct services and educational programs to help meet the needs of the craniofacial community, including:
(1) myFace Virtual Support Groups provide counsel and community for individuals and their families living with facial differences. These help participants to feel safe, supported, and never alone. myFace offers Support Groups for adults, adolescents, and both English-speaking and Spanish-speaking parents.
(2) Parent Guides provide resources and guidance to assist parents as they support their child’s journey.
(3) Transforming Lives Webinar Series offers webinars with craniofacial experts on topics of interest to the community.
(4) myFace, myStory Podcast Series offers monthly interviews and roundtable discussions on topics of interest to the craniofacial community.
(5) myFace’s Guide to Craniofacial Surgeries serves as a guide to patients’ surgical experience, providing in-depth information on 6 of the most common craniofacial surgeries.
(6) myFace’s Your Impact Newsletter provides in-depth quarterly updates for the community, while the myFace Email Listserv provides Monthly Updates and other communications about program outcomes, upcoming events, and more.
(7) myFace Apartments provide free housing for out-of-town families seeking treatment in New York City.
(8) myFace Wonder Project and school assemblies provides students with the tools they need to unite against bullying and to implement acts of kindness in their schools and in their communities.
(9) myFace Events provide opportunities for the craniofacial community to gather together.
References
- A guide to understanding hemifacial microsomia. Children’s Craniofacial Association. https://www.ccakids.org/assets/syndromebk_hemifacial.pdf. Accessed 6/25/22.
- Birgfeld CB, Heike C. Craniofacial microsomia. Semin Plast Surg. 2012; 26(2): 91-104. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3424699/
- Goldenhar syndrome. Cleveland Clinic. Reviewed 4/19/2022. https://my.clevelandclinic.org/health/diseases/22808-goldenhar-syndrome Accessed May 20, 2022.
- Goldenhar syndrome. Children’s Hospital of Philadelphia. https://www.chop.edu/conditions-diseases/goldenhar-syndrome Accessed May 21, 2022.
- Everything patients need to know about Goldenhar syndrome. HealthPrep.com. https://healthprep.com/articles/conditions/goldenhar-syndrome-overview/. Accessed May 21, 2022.
- Hemifacial microsomia/Goldenhar syndrome. Craniofacial Foundation of Utah. Accessed 6/24/22.
- Hemifacial microsomia. National Institute of Dental and Craniofacial Research. https://www.nidcr.nih.gov/health-info/hemifacial-microsomia. Accessed 6/25/22.
- Luquetti DV, Heike CL, Zarante I, et al. MYT1 role in the microtia-craniofacial microsomia spectrum. Mol Genet Genomic Med. 2020; 8:e1401.
- Oculo-auriculo-vertebral spectrum. NORD. https://rarediseases.org/rare-diseases/oculo-auriculo-vertebral-spectrum/. Accessed May 21, 2022.
- Stromland K, Miller M, Sjogreen L, et al. Oculo-auriculo-vertebral spectrum: associated abnormalities, functional deficits and possible developmental risk factors. Am J Med Genet A. 2007; 143A(12): 1317. (Full article online: https://pubmed.ncbi.nlm.nih.gov/17506093/)
- Taiwo AO. Classification and management of hemifacial microsomia: a literature review. Ann Ibd Pg Med. 2020; 18: S9-S15.
- Timberlake AT, Griffin C, Heike CL, et al. Haploinsufficiency of SF3B2 causes craniofacial microsomia. Nat Commun. 2021; 12: 4680. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8333351/
- Tuin J, Tahiri Y, Paliga JT, Taylor JA, Bartlett SP. Distinguishing Goldenhar syndrome from craniofacial microsomia. J Craniofac
- Surg. 2015; Sep 26(6): 1887-92. (https://pubmed.ncbi.nlm.nih.gov/26267577/)
- Syndromes with craniofacial abnormalities. UpToDate. Reviewed April 2021. https://www.uptodate.com/contents/syndromes-with-craniofacial-abnormalities Accessed May 21, 2022.
- Zielinski D, Markus B, Sheikh M, et al. OTX2 duplication is implicated in hemifacial microsomia. PLoS ONE. 2014; 9(5): e96788
In This Article
Click to jump to your selected section.