Treatments & Procedures for Cleft Lip and/or Palate
Home > Craniofacial Conditions > Cleft Lip and/or Palate > Treatments & Procedures
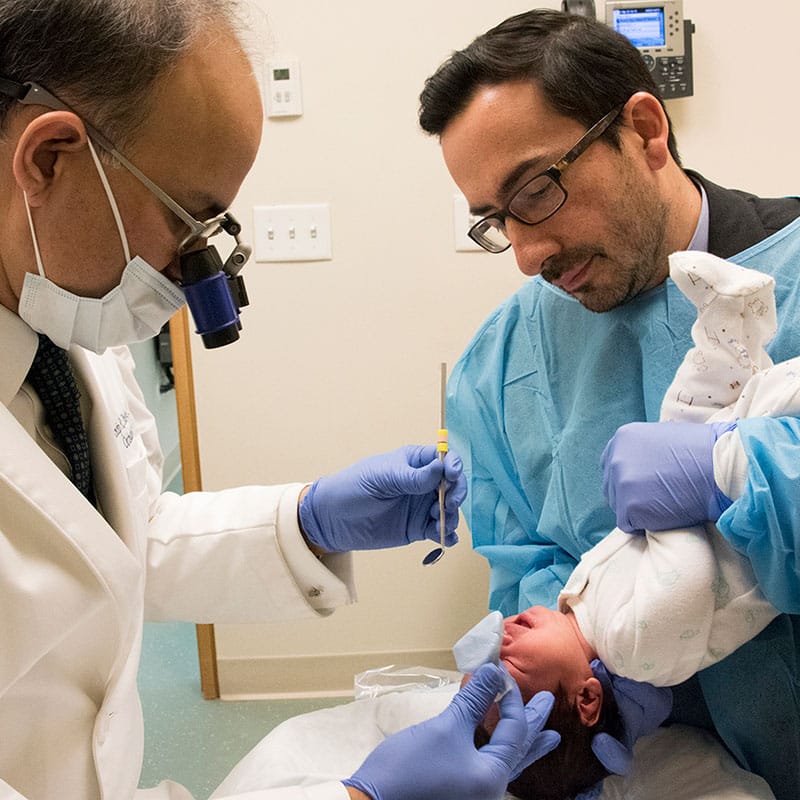
Surgery is the definitive treatment for clefts.
A child with a cleft lip/palate may require a variety of treatments and services depending on the severity of the cleft
The goals of treatment for the cleft(s) are to ensure normal breathing, feeding, hearing, speech and language development, and maxillofacial growth while preventing long-term complications. Surgery is the definitive treatment for clefts, but the preferred timing of the surgery may vary from center to center. Also, the specific surgery or technique used will depend on the type of cleft.
Procedures Used to Treat Cleft Lip and Palate
In general, procedures used to treat cleft lip/palate may include:
Presurgical Lip Taping
Babies with wide clefts may have their upper lip reshaped through taping. The goal of taping is to make the cleft smaller prior to surgery. Family members are given instruction and a demonstration in the clinic on how to place tape across the cleft under tension. Taping does not interfere with feeding, and can be used up until the time of cleft lip surgery. Taping may be combined with Nasoalveolar Molding for infants with wider clefts.
Presurgical Nasoalveolar Molding (NAM)
NAM is a custom appliance that is fitted by an orthodontist to help reshape the gums, lip, and nose prior to surgery. NAM treatment begins as soon as possible – often as early as the first week of life. The baby wears the NAM device 24 hours a day, and its shape gently redirects the growth of the upper jaw and gums. During this time, the baby visits the orthodontist every week to make adjustments to the NAM device. The molding can reduce the size of large or wide clefts and can therefore potentially decrease the number of surgeries that the child will need to undergo. The mold can improve the shape and position of the lip and nose.
Surgical Lip Adhesion
In cases of wide or bilateral cleft lip, lip adhesion may be performed between 6 weeks and 3 months of age as the first step in a two-stage approach to lip repair. During the procedure, the surgeon stitches the two sides of the cleft together. The purpose of the lip adhesion is to reduce the tension on the final repair, which might result in a narrower scar. Some surgeons might also request that parents tape the upper lip prior to the adhesion to help narrow the cleft even before lip adhesion surgery. The second stage of this process involves further realignment of the lip.
Cleft Lip Surgery
This procedure, typically done between 3-6 months of age, involves closing of the separated lip tissues. There are a variety of techniques that may be used to repair a cleft lip. The plastic surgeon creates flaps of tissue from both sides of the cleft lip and then stitches them together. If the cleft extends into the nose, the initial nasal repair is also done at this time.
Cleft Palate Surgery
The goal of this surgery is to fix the roof of the mouth so that the child can eat and talk normally. This is generally performed by 9-12 months of age, and sometimes earlier. There is no consensus on the best time to perform palate surgery. Earlier palate surgeries may have better speech outcomes, whereas delaying surgery may allow for more growth prior to surgery. Palate surgery involves closing of the separation and reconstruction of both the hard and soft palates, depending on the extent of the cleft. The surgeon moves tissue from the intact sides of the roof of the mouth to the center where the cleft is located, and the muscles of the soft palate are repositioned to help with proper speech development. A variety of different techniques may be used to repair the palate. Palate repair not only closes the palate – it also realigns the palate muscles so that they are in a good position for eating, swallowing, and speech. After the initial repair, about 30-40% of children with cleft palate will need additional surgeries to further improve their speech.
Ear Tube Placement
Children with cleft palate are more prone to ear infections and hearing loss due to fluid buildup in the middle ear. Thus, doctors may recommend that special tubes be placed in their ears to help fluid drain more easily. This is often done at the same time as the palate repair.
Speech Therapy
Almost half of all children with cleft palate will need some form of speech and language therapy. Children with a cleft that affects their soft palate may have speech that has a nasal quality to it. This occurs because the soft palate is not able to properly close off the mouth from the nose when speaking, which lets air escape through the nose. Children who still have holes (fistulas) in the palate may have difficulty producing some consonants. And if teeth are missing or not in the right place, a child may have difficulty articulating dental sounds, such as f and v. Speech issues should be picked up and managed by a child’s Cleft Team. Children are assessed for speech impairment around 18-24 months of age and again at 3 years of age. The aim is for children to have good quality speech by age 5-6 so that they can enter school fully prepared to communicate clearly.
Palate Expansion
Children with cleft palate tend to have a narrow and collapsed palate, which can be problematic for proper development of adult teeth. A palate expansion is a procedure done by an orthodontist, in conjunction with a plastic surgeon, to place an expander device into the child’s upper jaw, typically at the age of 5 to 7, when the child’s permanent teeth are beginning to develop. This device is then expanded gradually over several months to widen the jaw. This results in better alignment of the upper and lower jaw and makes more room for adult teeth.
Alveolar Bone Graft
The purpose of the surgery is to add bone to the alveolus (the gum ridge that holds the teeth). This is a common procedure that is performed before the permanent teeth come in, which usually happens between ages 8 to 10. The oral maxillofacial or plastic surgeon will remove a small amount of bone from the child’s hip. The surgeon will then open the gum line around the cleft, place the harvested bone into the gap, and close up the incisions with sutures.
Pharyngoplasty
Children with a cleft palate may sometimes have a short soft palate, poor palate function, or both. As a result, the soft palate does not properly separate the back of the mouth from the nose during talking, resulting in nasal-sounding speech and abnormal air leakage through the nose while speaking. A pharyngoplasty is a surgery that takes tissue from behind the tonsils, attaches it to the back of the throat to narrow the space behind the palate, and prevents air from leaking through the nose while speaking.
Orthodontics
Children with clefts often have problems with missing, malformed, or poorly positioned teeth. Thus, it is important to involve an orthodontist even before the child has any teeth to assess facial and jaw growth and development and to anticipate short and long-term dental needs. After the permanent teeth grow in, the orthodontist may use braces or other techniques to straighten and reposition the teeth.
Orthognathic (Jaw) Surgery
Children with cleft lip/palate often have an underdeveloped upper jaw (maxillary hypoplasia), especially after the cleft repairs that are done during the first year of life. Orthognathic (jaw) surgeries are typically done in the late teen or early adult ages to stabilize and straighten the jaw. Orthodontic treatments are often required in preparation for jaw surgery.\
Distraction Osteogenesis
This is a technique that may be used to elongate the bones of the jaw and midface. During surgery, the short bone is cut (an osteotomy), and a device called a distractor pulls the bone apart slowly, allowing new bone to grow (osteogenesis) to fill the gap. The titanium distractor can be placed in a variety of ways, including under the skin, attached to the skull and face bones, or on the outside of the skin. After surgery, the distractor is adjusted 1-2 millimeters per day to move the bones apart, while the new bone develops to fill the gap. Once the bones are in the desired position, they are allowed to heal and consolidate; this phase lasts 1-2 months.
Cleft Rhinoplasty
These surgeries are typically done during the later teen years, when children are done growing. Lip revision can improve the symmetry and fullness of the lips, reduce visibility of scarring, and improve the thin appearance of the upper lip. A nose revision (or rhinoplasty) can help to correct uneven nostrils, relieve nasal airway obstruction, straighten the nose, and reshape the tip of the nose.
Follow-up surgeries
Follow-up surgeries (between age 2 to late teen years) may include additional reconstructive surgeries to improve the appearance of the lip, nose, or mouth. Other surgeries may also be required to prevent or treat related complications.
Surgery for cleft lip and palate can result in significant improvements in appearance, ability to eat, breathe, and talk. However, if the cleft is severe or treatment is inadequate, patients may still be left with some challenges including compromised appearance and speech difficulties. Also, families should be aware of common surgical complications including bleeding, infection, worsening scars, and possible damage to nerves and other structures.
Resources for the Craniofacial Community
myFace provides individuals and families living with a facial difference access to holistic comprehensive care, psychosocial services, education, resources and support that pave the way for better outcomes.